(July-2023) Unlocking the Potential of Value-Based Care by Accelerating Access to Specialty Medical Care In today’s rapidly evolving healthcare landscape, value-based care has emerged as a game-changer. By prioritizing patient…
read more(May-2023) Most providers have around 5% unbooked appointment slots every month. If every specialist made 5% of their weekly work schedule available for extra appointments and those unbooked appointment slots…
read more(Mar-2023) With 24/7 internet access and unprecedented access to information, patients are a lot more selective when finding and choosing a healthcare provider. 90% of people do some kind of…
read more(Feb-2023) Last year, our managed specialty physician network reached thousands of patients spread across 27 states. Each month, thousands of patients spend over 6 minutes per visit on the nodMD.com…
read more(Jan-2023) Three years ago, nodMD was founded to reduce patient wait time to see a U. S. specialty physician by up to 25%. Specialty care physicians in our managed network…
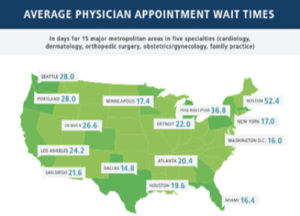
read more(Nov-2022) A decrease in the number of active specialists along with an increase in the aging U.S. population has increased average wait times for new patients to see a U.…
read more(Oct-2022) Over 40 million new patients see a specialty physician every year and for many, finding the right specialist can be challenging. Patients are increasingly engaged in their health journey. …
read more(Aug-2022) Every day, an average of 1 in 25 hospital patients (United States) contracts at least one healthcare associated infection (HAI), according to the CDC. HAIs include: pneumonia, surgical site…
read more(July-2022) Patients want to be engaged in their health journey. They want a provider with online booking and they want to schedule an appointment with the same ease as scheduling…
read more(Jan 2021) “Telemedicine is an essential tool for physicians and healthcare providers to provide care and treatment using telecommunication technology.” We couldn’t have said it better ourselves, but credit where…
read more(Oct 2020)Thursday, October 8th, 2020 • apic.org/cds2020 Are you an infection preventionist at a rural community hospital or ambulatory surgery center that is planning on attending the Cleaning, Disinfection, and…
read more(Jul 2020) nodSpecialists Brings Mobile Lab To Patients Homes for COVID-19 Testing In Arizona and Colorado FOR IMMEDIATE RELEASE (PHOENIX – July 14, 2020) – Infectious disease provider Nod Specialists…
read more- 1
- 2